Vascular Surgery Team
Collaboration with vascular surgery specialists
Vascular access is a critically important factor for the proper and effective treatment of dialysis patients, ensuring their optimal health and well-being.
The Nephrology Center Nefrontida collaborates with a team of experienced vascular surgeons, who undertake the creation of new vascular access (fistula or graft) and the placement of temporary or permanent venous catheters for hemodialysis.
In addition, our team of collaborating vascular surgeons undertakes corrective interventions on vascular access, such as thrombectomy and angioplasty of arteriovenous grafts, restoration of malfunctioning arteriovenous fistulas, as well as angiographic studies in cases of dysfunctional vascular access.
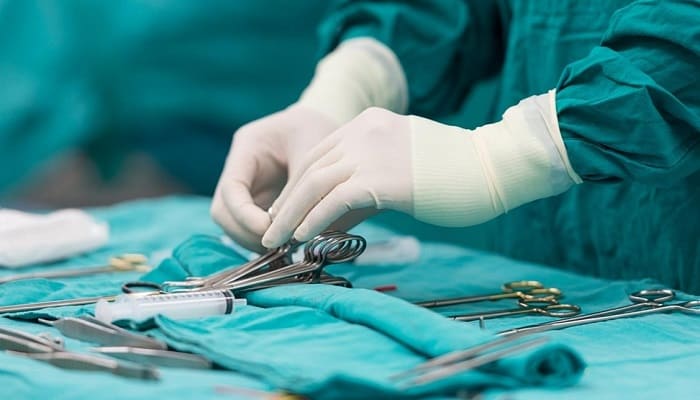

Our Center’s Policy on Vascular Access
Patients monitored in our Center’s outpatient clinics by our Nephrologists who are in the pre-dialysis stage of chronic kidney disease are ensured timely referral to our collaborating vascular surgeons for ultrasound vascular assessment, mapping, and timely creation of arteriovenous access.
The timely creation of vascular access is especially important as it allows for necessary corrective interventions before its use, in case the access does not show signs of adequate development. This way, when clinical and laboratory indications require the start of hemodialysis, the patient already has a mature vascular access, enabling a planned and smooth initiation of treatment.
Our Center dialysis patients', vascular access is monitored on a daily basis. This monitoring is performed using ultrasound within the Unit by both our experienced nursing staff and the Center’s nephrologists. Monitoring takes place, both, before cannulation and during treatment. In this way, a successful and safe cannulation of the vascular access is ensured, as well as adjustment of the needle position within the vessel during treatment when indicated by the hemodialysis machine.
Timely vascular surgical corrective intervention: Through systematic monitoring of vascular access, issues such as stenosis at the anastomosis site or along the vessel, or early thrombosis, are identified promptly. This ensures timely vascular surgical corrective intervention, thereby achieving long-term survival of the vascular access and minimizing patient discomfort.
“Less than 15% catheter” policy: Our Center aims to maintain the percentage of hemodialysis catheters within the Unit at below 15% of our patients. This is achieved through the timely creation of vascular access in patients starting dialysis and proper monitoring to prevent thrombosis and loss of access. Thus, the use of central venous catheters as vascular access for hemodialysis is limited only to patients for whom arteriovenous access is not feasible after vascular surgical evaluation, and to patients who begin hemodialysis with the prospect of a soon kidney transplant from a living donor.

